|
Keep in mind the two most basic formulas in respiration: P aO2 = P iO2 - P CO2/R and P aCO2 = V CO2/V AxK When the patient was given 27% O 2 to breath his P aO2 rose to ~100 mm Hg. Blood gas analysis obtained with the patient breathing room air showed a P aO2 of 50 mm Hg and a P aCO2 of 80 mm Hg. The effect of hypoventilation on alveolar and system arterial P CO2 and P O2 will be illustrated an example of a man with normal lungs who takes an overdose of barbiturates which depresses his medullary respiratory center, such that alveolar ventilation is depressed by half while CO 2 output remains normal. 
The most common cause of hypoventilation is depression of the medullary respiratory center by drugs. Clinically, the hallmark of inadequate ventilation is hypercapnia, an elevated systemic arterial P CO2 (P aCO2 > 43 mm Hg). Hypoventilation: Hypoxemia develops when the pulmonary alveoli are inadequately ventilated. Read Chapter 5 of West, Respiratory Physiology 7th ed.Ībnormally low oxygen in the blood is caused by one or more of the following: (1) Hypoventilation (2) diffusion impairment (3) right to left shunt (usually in the lungs, but can be in the heart) (4) abnormal ventilation/perfusion ratios. Lisa Ebihara MD-PhD, Department of Physiology and Biophysics 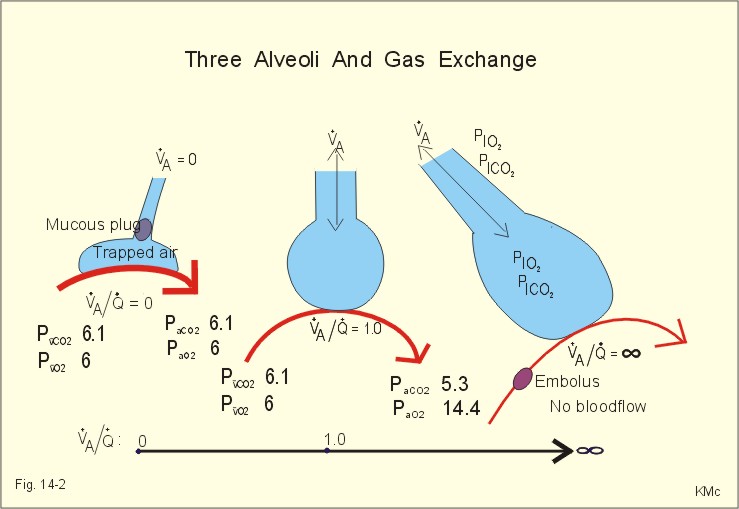
Four causes of hypoxemia: Abnormal ventilation/perfusion ratios as the major cause of hypoxemia.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
